References
Preventing urinary tract infection and supporting patient catheterisation for mental health
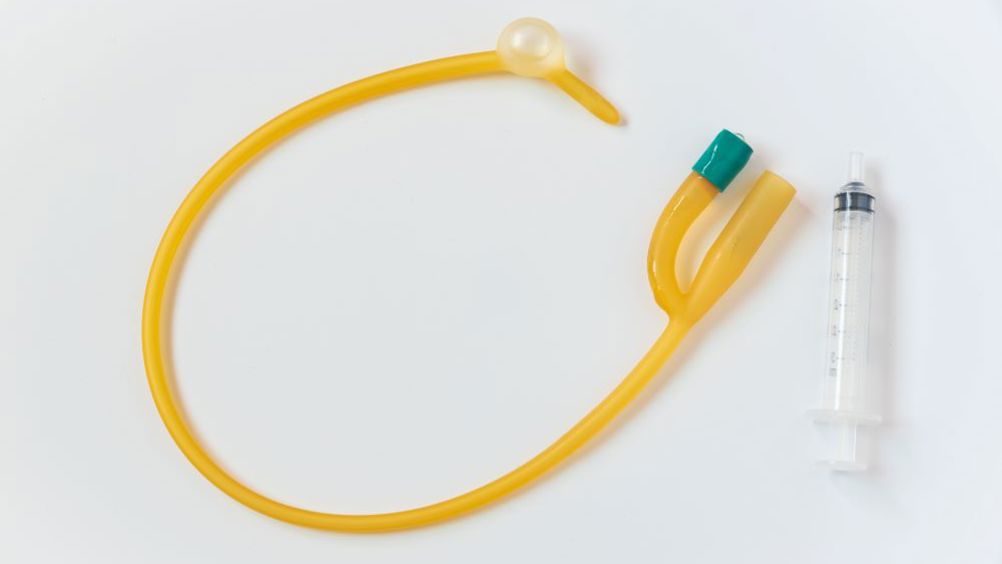
Research has revealed uncertainty among catheter users about the signs and symptoms of urinary tract infection (UTI) and at what point they should seek help (Okamoto et al, 2017). In this study, the researchers recommended development of a self-help tool for patients that could assist with the identification of infection, as well as improve communication between patients and health professionals. The tool could prevent excessive or unnecessary contact with practitioners by ensuring that patients have the tools and abilities to self-manage, while providing the knowledge for patients to know when it is time to seek help.
A tool has been developed that requires a health professional to carry out the assessment (Lauridsen et al, 2022). A UTI risk factor model was used as the basis to inform the content included in the tool and the authors used the Design Thinking Process to guide its development, in terms of its content and format.
Register now to continue reading
Thank you for visiting Journal of Prescribing Practice and reading some of our peer-reviewed resources for prescribing professionals. To read more, please register today. You’ll enjoy the following great benefits:
What's included
-
Limited access to our clinical or professional articles
-
New content and clinical newsletter updates each month

